The History of Influenza
Deadly pandemics, health crises, scientific discoveries, vaccine innovations and disease prevention.
Explore a historical timeline of major influenza events.
Scroll to Begin

Origin
Before 1600AD
Prehistory
Origins of influenza
When did the influenza virus first infect humans? Some scientists hypothesize that humans probably acquired influenza when they began domesticating animals like birds and pigs. The rise of agriculture and permanent settlements provided ideal conditions to trigger a flu epidemic.
Region: Global
Did you know?
When an infectious disease becomes zoonotic, it can jump from a non-human animal to a human. Contact with domestic, agricultural or wildlife animals can sometimes transmit deadly pathogens and trigger an outbreak.
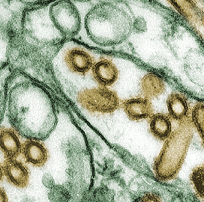
Electron micrograph of avian influenza.
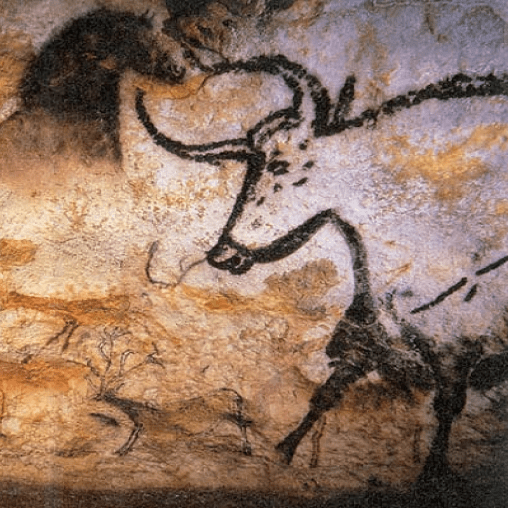
Cave paintings from Lascaux caves depicting animals during prehistoric times.

Engraved bust of Hippocrates.
412BC
Early evidence of influenza
While the flu has most likely been around for ages, no definitive historical records exist.
In his sixth book of “Epidemics,” the Greek physician Hippocrates describes a highly contagious disease with flu-like symptoms. Modern doctors believe this may be the first reference of influenza (412BC).
Region: Europe

Miniature of Richard of Wallingford, Abbot of St. Albans, mathematician and inventor of a mechanical astronomical clock.
1357
“La influenza” is coined
La influenza comes from Italian, meaning "visitation" or "influence."
In 1357, people called an epidemic in Florence, Italy “influenza di freddo,” which translates to “cold influence.” This may be a reference to the possible cause of the disease.
Many astrologers in the Middle Ages believed that the periodic return of the disease was related to the "influence of heavenly bodies" or "influenza di stelle," meaning "influence of the stars."
Region: Europe
1580
The first flu pandemic
Most epidemiologists agree that the 1580 influenza outbreak is the earliest recorded flu pandemic. It began in Asia during the summer before spreading to Africa, Europe, and eventually across the seas to the Americas. While the total death toll is unknown, it killed 8,000 people in Rome.
Region: Global
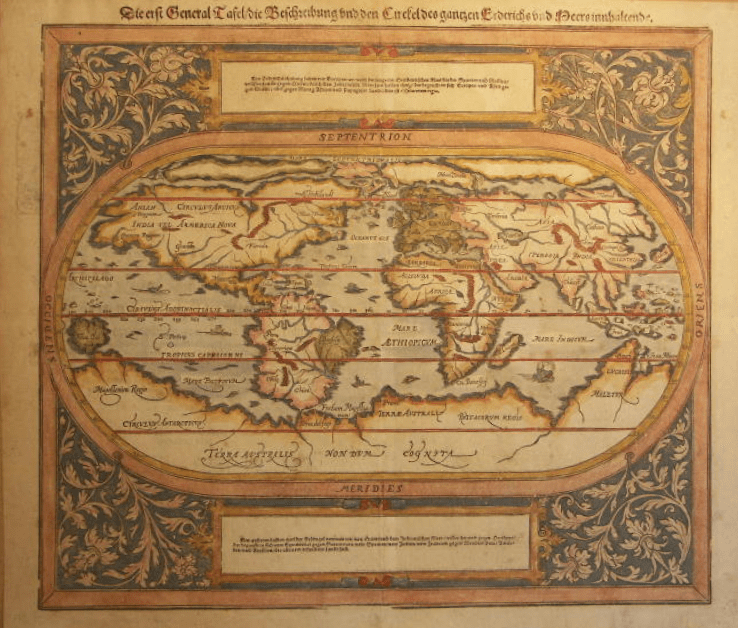
Münster's maps, 1580.
18th to 19th Century
Pandemics
1700–1899
1729
The first influenza pandemic of the 18th century started in Russia. It spread throughout Europe within six months and the world within three years.
Region: Global
1781
After starting in China, this influenza outbreak spread to Russia, eventually reaching Europe and North America over the next year. At the height of the pandemic, 30,000 were infected every day in St. Petersburg.
Region: Global
1830–1833
This pandemic spread by ships from China to the Philippines, India and Indonesia. After crossing Russia to Europe, it eventually reached North America. While the mortality rate was low, the flu pandemic between 1830 and 1833 impacted 20%–25% of the population.
Region: Global

The Honourable East India Company's Ship Inglis leaving St Helena in July 1830.
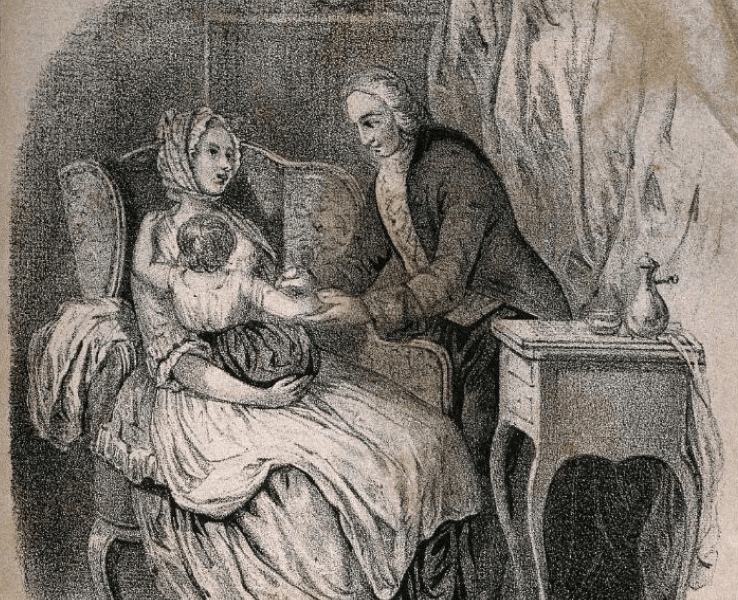
Edward Jenner vaccinates a young child on its mother's lap.
1796
The world's first vaccine
Can an infection from cowpox produce immunity to smallpox?
On May 14, 1796, British physician and scientist Edward Jenner tested this hypothesis and pioneered the first vaccine. Jenner inoculated an 8-year-old boy named James Phipps with pus scraped from cowpox blisters on a milkmaid's hands. The boy fell ill with a mild case of cowpox but fully recovered. In July, Jenner inoculated Phipps with scabs of smallpox. The boy remained healthy and had developed immunity.
Jenner's method was eventually called vaccination. “Vacca” is the Latin word for cow.
Region: Europe
Did you know?
Inoculation has been around for hundreds of years. There’s evidence that the Chinese and Indians used smallpox vaccination as early as the 16th century.
1879
First laboratory vaccine
Louis Pasteur produced a vaccine for chicken cholera called Pasteurella Multocida. It is celebrated as the first laboratory-developed vaccine.
Pasteur was studying fowl cholera and injecting chickens with live bacteria. He accidentally stumbled on a great scientific discovery when his assistant left out a fresh culture of bacteria over a holiday. Upon their return to the lab, Pasteur discovered exposure to oxygen weakened the bacteria so that chickens could survive infection and develop immunity.
Region: Europe

Portrait of Louis Pasteur.

Louis Pasteur performing an experiment.
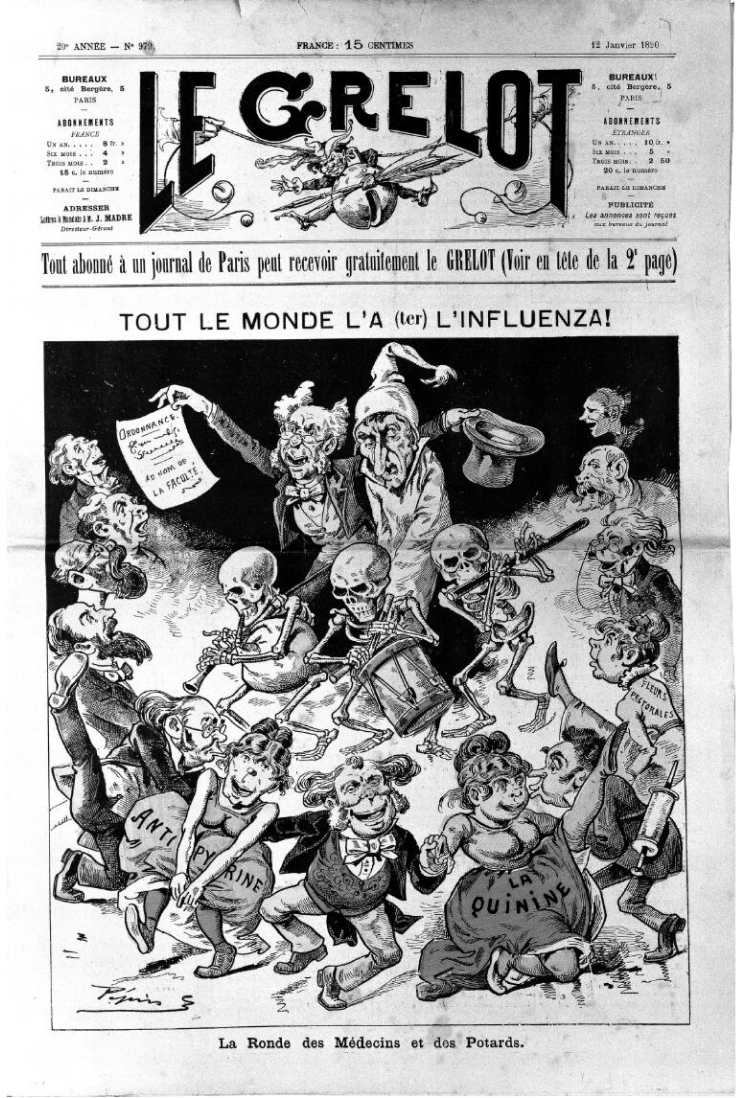
Political cartoon referring to the influenza epidemic in Paris and Europe.
1889
First modern flu pandemic
One of the deadliest pandemics in history, the so-called Russian Flu infected 40% of the world’s population and killed about 1 million people. While it’s the last flu pandemic of the 19th century, it is the first to rapidly spread around the whole world due to the modern transport infrastructure of railroads and transatlantic sea travel.
Region: Global
20th Century
Spanish Flu
1918–1919
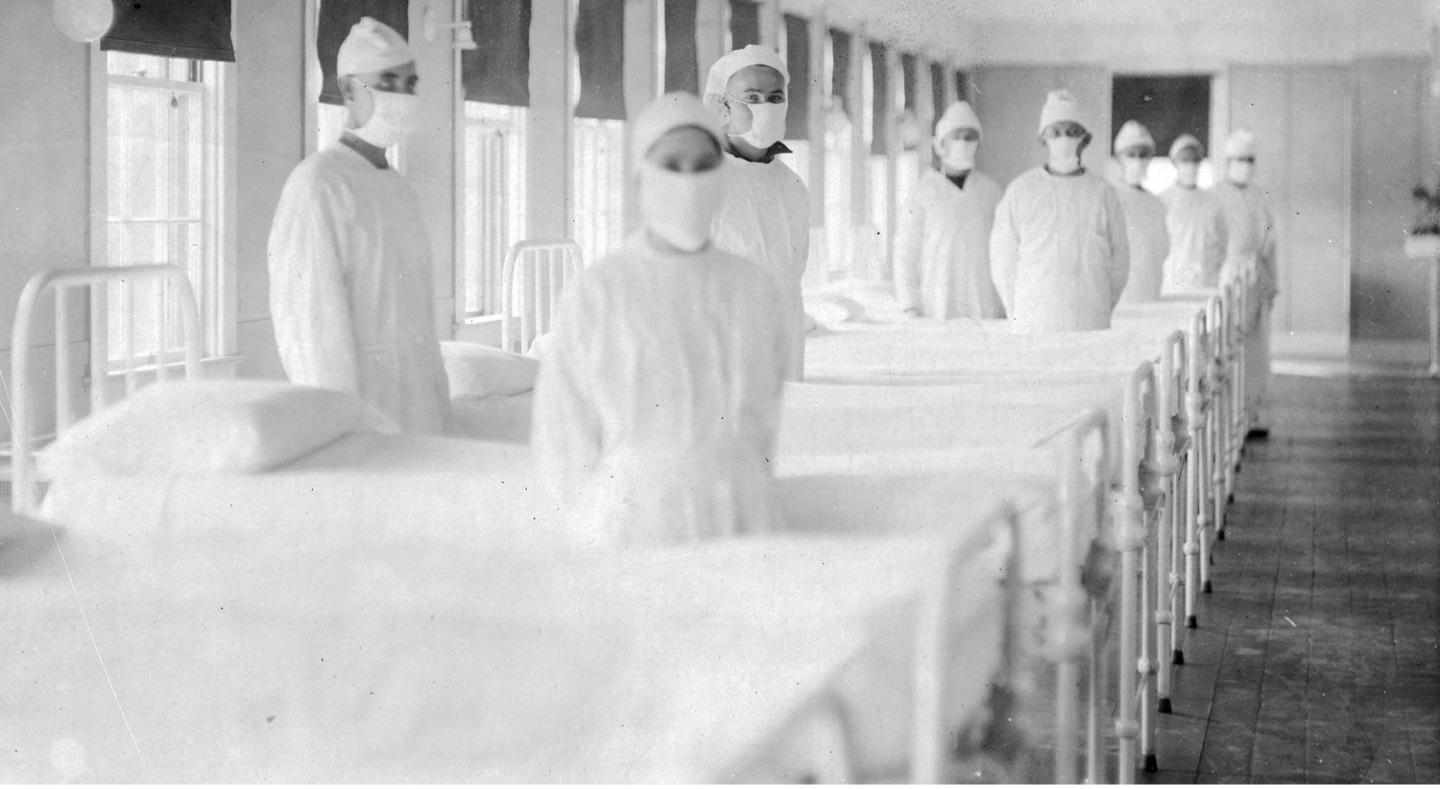
Corpsmen in caps and gowns ready to attend patients in the influenza ward of the U.S. Naval Hospital on Mare Island, Calif., on December 10, 1918.
1918
The deadliest pandemic of the 20th century
The 1918 influenza outbreak was caused by a new strain of the influenza A virus that started in birds (H1N1).
After reports in Europe, Asia and the United States, it rapidly spread around the world. About one-third of the world’s population was infected and 20 million to 50 million people were killed.
The average life expectancy in the United States dropped by about 12 years.
Region: Global
1918
Halting the spread
At the time, there were no vaccines or drugs to treat influenza. People got very sick, very quickly. Hospitals were overwhelmed. Many communities imposed quarantines and closed churches, schools, and public spaces. The public used gauze masks to stop the spread of the disease.
Region: Global

Newspaper article (The Washington Times, September 27, 1918) showing gauze mask recommended by the Red Cross to halt spread of the Spanish Flu.

1918 influenza epidemic poster issued by the Board of Health in Alberta, Canada.
1918–1919
Protecting the public health
How do you control a deadly contagious disease in an era of mass transportation, crowded cities and world war?
Implementing social distancing measures played a big role in reducing the spread. Cities that acted early and sustained preventive measures longer suffered lower death rates.
Region: Global
20th Century
Scientific Discoveries
1933–1952
1933
Influenza virus isolated
The significant losses endured in the 1918–1919 pandemic inspired a period of great scientific research and discovery. In the 1920s, some scientists started to suspect that bacteria were not the real cause of influenza disease.
In 1933, scientists at the National Institute for Medical Research in London isolated the influenza A virus from nasal secretions of infected human patients. This discovery would lead to the innovation of inactivated vaccines in the late 1930s and 1940s.
Region: North America
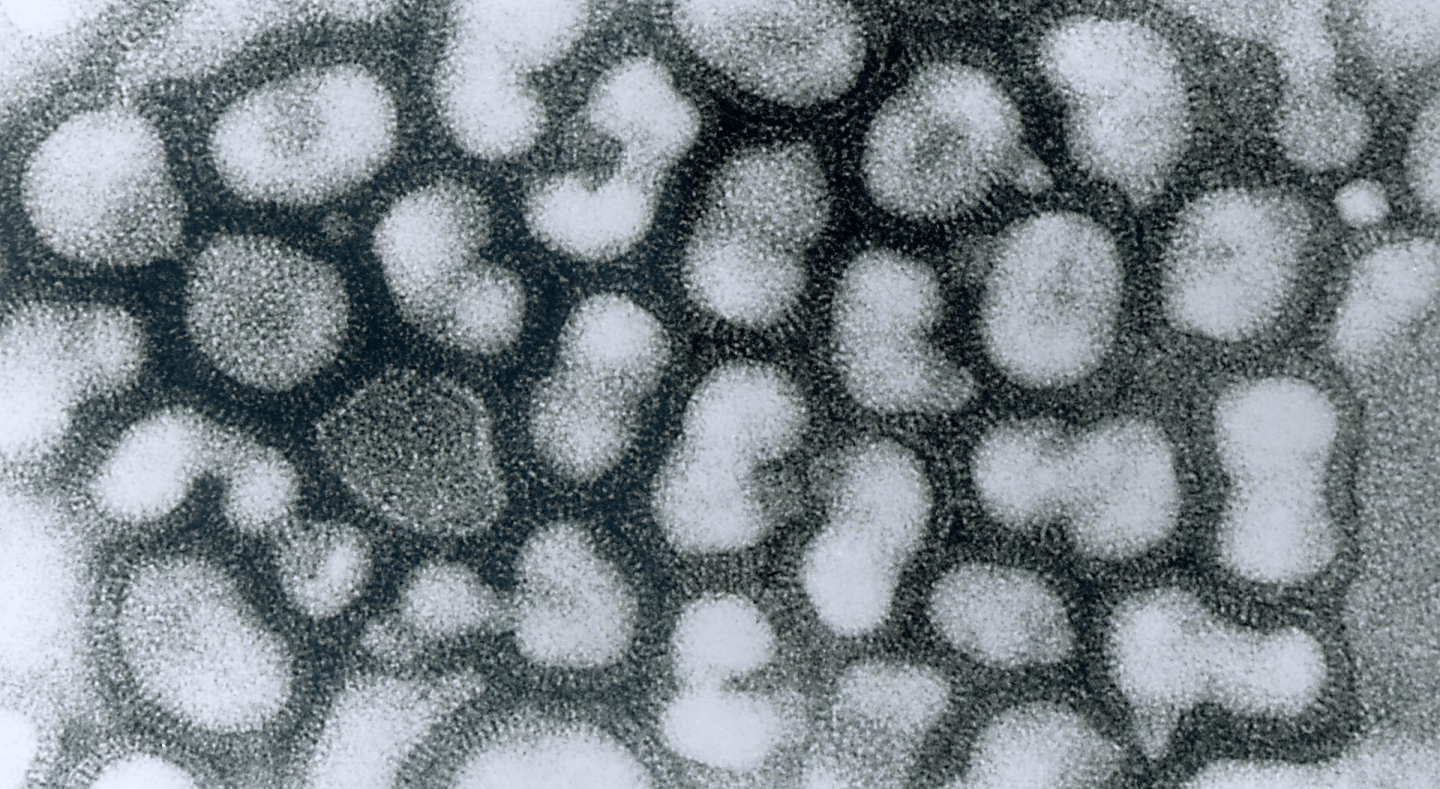
Transmission electron micrograph of influenza A virus.

U.S. Army hospital ship at Cherbourg, France, harbor, May 22, 1945.
1945–1946
Influenza vaccine approved
The immense loss of soldiers during the 1918 pandemic made the flu vaccine a priority for the U.S. military. The development of the first inactivated flu vaccine was led by Thomas Francis, Jr., and Jonas Salk of the University of Michigan. Their vaccine used fertilized chicken eggs — a method still used today to produce most flu vaccines. The first influenza vaccine was approved in the United States for military use in 1945 and civilian use in 1946.
Region: North America
1952
WHO creates first system for surveillance
During the seasonal flu epidemic of 1947,
small changes in the composition of influenza viruses had made existing vaccines ineffective.
The World Health Organization (WHO) Influenza Centre was established in 1948 to identify new influenza viruses and
control the spread of disease.
In 1952, the WHO launched the first system for the surveillance of circulating influenza virus strains.
This helped researchers to determine the composition of seasonal influenza vaccines.
Region: Global

Eggs have been used to manufacture seasonal flu vaccines for over 70 years.
20th Century
Asian and Hong Kong Flu
1957–1970
1957
Asian Flu pandemic
A new influenza A virus struck East Asia in 1957, unleashing a devastating global pandemic. First reported in Singapore, it quickly spread to Hong Kong in April and the United States by summer. The estimated number of deaths was 1.1 million worldwide and 116,000 in the United States. The rapid development of a vaccine and the availability of antibiotics limited the spread and death toll.
Region: Global

Asian flu hits the Vivallius School in Örebro. Barbro Ogenvall teaches a nearly empty classroom.
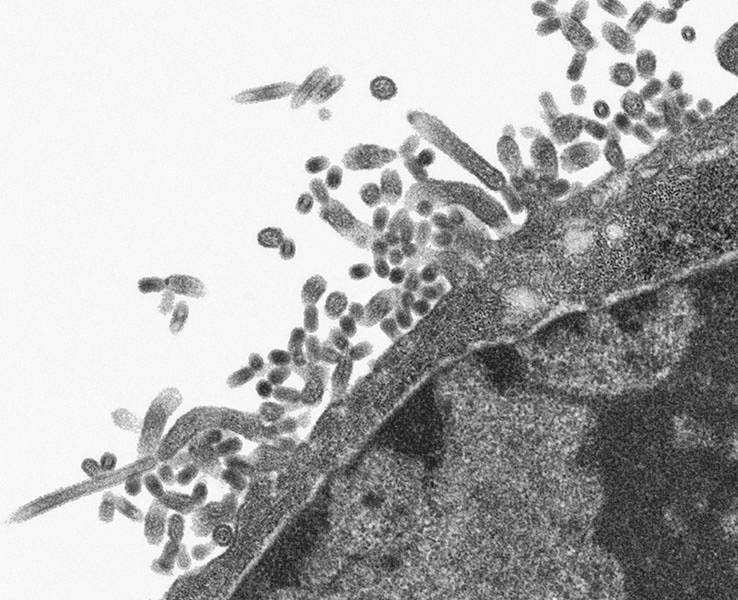
Microscopic view of influenza virus.
1968–1970
Hong Kong Flu
The 1968 global outbreak of influenza originated in China. The virus was highly contagious — in Hong Kong, 500,000 cases of illness were reported within two weeks. It quickly spread throughout Southeast Asia and reached the United States within months, transported by soldiers returning from Viet Nam.
Experts suspect that it evolved from the strain of influenza that caused the 1957 pandemic. Many exposed to the 1957 virus retained immunity against the 1968 virus. The pandemic killed between one and four million people globally.
Region: Global
20th to 21st Century
Innovations
1963–2012
1963
Idoxuridine, the first antiviral drug, was approved. Since this scientific breakthrough, antiviral drugs have helped millions people around the world.
Region: Global
1978
Scientists developed the first trivalent flu vaccine, which protected against three different strains of influenza. Today, quadrivalent flu vaccines are commonly used every flu season to protect against four different flu strains.
Region: Global
Did you know?
The Messenger RNA (mRNA) vaccines teach our cells how to make a protein that will trigger an immune response inside our bodies.

Scientist conducting medical research in a laboratory.
Computer illustration of a molecular model of messenger ribonucleic acid (mRNA).
1993
The first study is published demonstrating mRNA vaccination in mice.
Region: Global
2009
Swine Flu
A new influenza H1N1 virus was detected in the United States in April 2009 before quickly spreading worldwide. Swine flu primarily affected children and young adults who had no immunity to the new virus. There were 60.8 million cases and and 12,469 deaths in the United States alone. Due to the rapid response of the CDC and WHO, a vaccine was quickly developed. The first doses were administered on October 5 of the same year.
Region: Global
- 50,000+ confirmed cases
- 5,000+ confirmed cases
- 500+ confirmed cases
- 50+ confirmed cases
- 5+ confirmed cases
2012
New studies show that mRNA vaccines induce long-lived and protective immunity to influenza.
Region: Global

Doctor administers a vaccine shot.
21st Century
Beyond Flu to Coronavirus
2020–Present

Scientist studying samples under a microscope.
2020–2021
Flu vaccine effectiveness, COVID-19 vaccine development
Between 2019 and 2020, flu vaccines prevented about 7.5
million illnesses, 3.7 million doctor visits, 105,000 hospital stays and 6,300
deaths in the U.S. alone.
In January 2020, scientists began work on the vaccine in response to the COVID-19 pandemic. Because organizations like the National Institutes of Health (NIH) have been researching coronaviruses for years, scientists were able to innovate much faster. On August 23, 2021 the U.S. Food and Drug Administration approved the first COVID-19 vaccine.
Region: Global
The Future
Smarter vaccines
How do you create a better flu vaccine?
Researchers have been exploring new mRNA vaccine technology which can provide biological instructions for cells to produce proteins that trigger an immune response.
A mRNA influenza vaccine could enable a faster response to outbreaks and potentially save more lives.
Region: Global

Rows of test tubes in a research laboratory.
